Health Journal
Browse the Medmate Journal
Search for a specific topic or filter by categories to find information on what you need to know.

What Are Antihistamines and How Do They Work?
If you experience sneezing fits in spring, itchy skin after contact with something new, or watery eyes around pets, you may have been told to take an antihistamine. But what…

Why Australia Needs Always-Available Healthcare — And How We Are Building It
By Dr Ganesh Naidoo, Medical Director, Medmate Australia’s health system is standing at a genuine inflection point. The release of the National Digital Health Strategy Action & Impact Report reflects…

The Belt Squat RDL is a Game-Changer
Looking to build a stronger, more powerful lower body while minimizing risk? The Belt Squat RDL might just be the exercise you’ve been missing. This unique movement, often overlooked, offers…

Why Akkermansia Might Be the Coolest Gut Bacteria You’ve Never Heard Of
At Medmate, we’re always learning about the latest science to help people feel their best.One of the coolest discoveries? A special gut bacteria called Akkermansia muciniphila (you can just call…
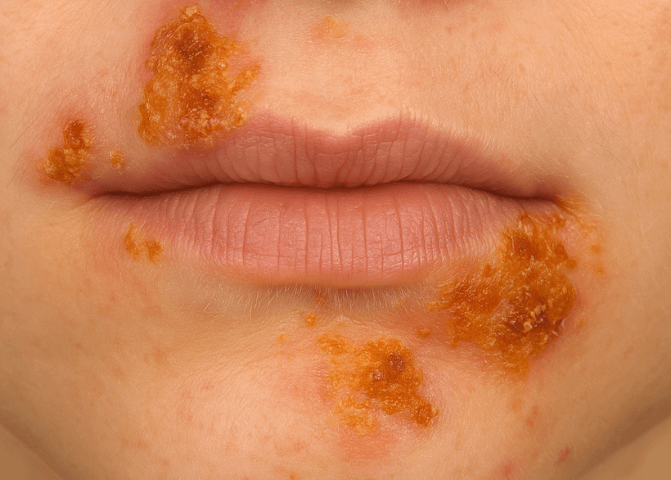
Impetigo (School Sores): Your Complete Parent Guide
Impetigo, often called school sores, is a highly contagious bacterial skin infection affecting millions of children each year. This common childhood condition shows up as red sores or blisters that…
Medical Certificate Backdating in Australia: Your Complete Guide
At Medmate, Australia’s trusted 24/7 telehealth service, we know medical certificates can sometimes be confusing — especially when people ask about “backdating.” The important point is this: the issue date…